.webp)
.webp)
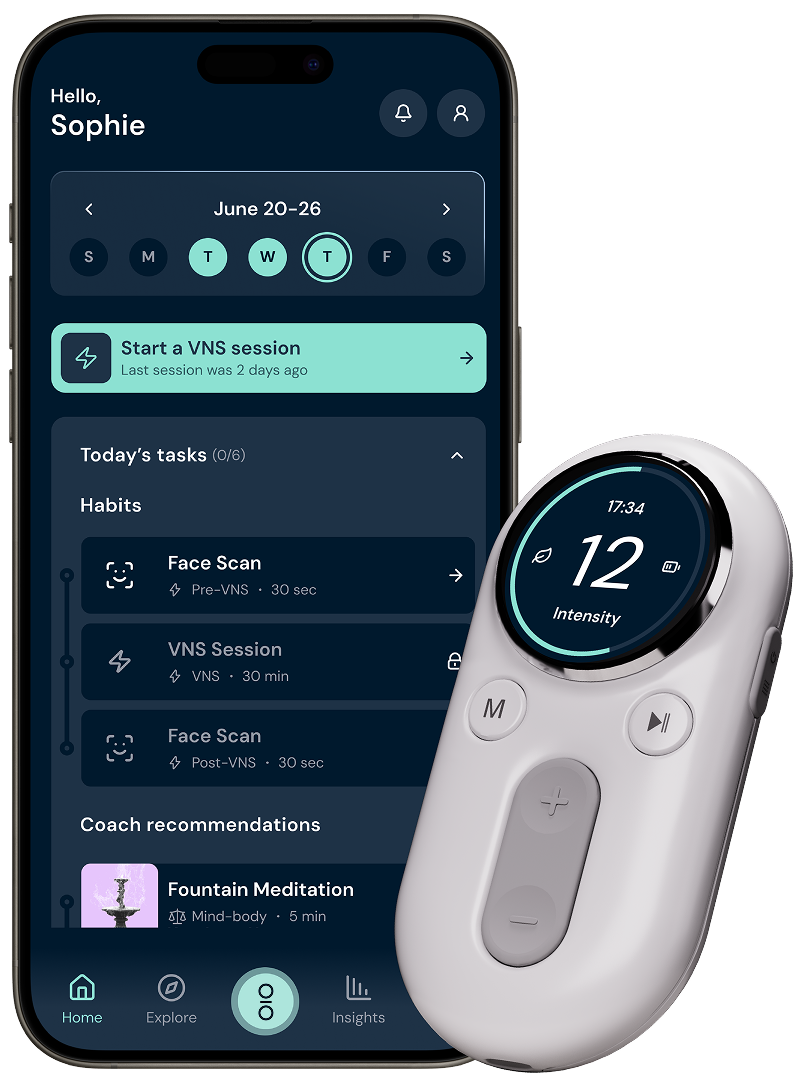
Your personal path to feelingYour personal path to feelingunshakeableunshakeabletodaytomorrowand beyondtoday
Using personalized programs, biotech, real-time biofeedback, and expert support, we help you get back to your best… and stay there.

Difference
Your everyday vitality, supported
yōjō’s wellness ecosystem breaks the stress-inflammation cycle and nurtures lasting psychological, physiological, and social well-being.
Testimonials
Real people, real results
What yōjō members say a few weeks after partnering with yōjō.
Benefits
A guided journey for lasting health and vitality
Our whole-person approach strengthens your nervous system, helping you stay calm, resilient, and ready.




Stress relief
yōjō calms your mind and body, lowering stress hormones and restoring balance so you feel more in control.
.webp)
Sharper focus
yōjō supports healthy brain activity, boosting attention, memory, and clarity, so you can stay focused when it matters most.
.webp)

Deeper sleep
yōjō helps your body switch into rest mode, making it easier to fall asleep, stay asleep, and wake up refreshed.
.webp)


Steady energy
yōjō restores efficient energy use in your body, giving you steady fuel for your day without the slump.

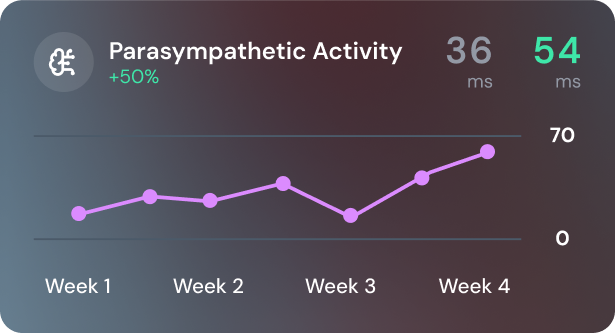
Faster recovery
yōjō resets your system, speeds recovery, and restores vitality, helping you train harder, perform better, and bounce back sooner.
.webp)

Better mood
yōjō nurtures the mind–body connection, reducing stress and inflammation’s impact on gut health and immune function, so you feel lighter, brighter, and more resilient.
How It Works
A small daily ritual that helps you do you better
Follow your personal program to balance your nervous system, build stress tolerance, and live your best life.
.webp)
.webp)
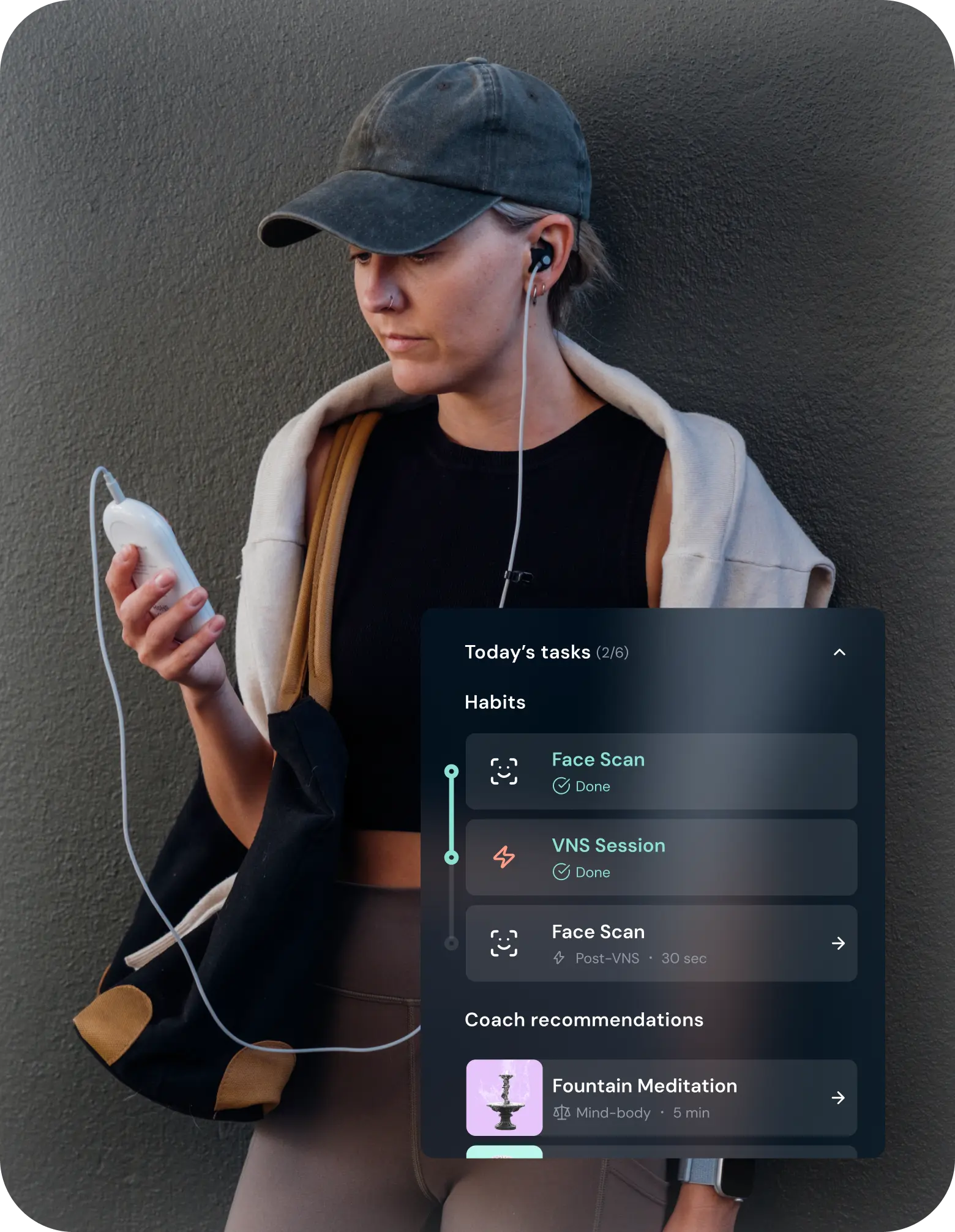

Scan
Activity
Scan
Results
Capture health metrics before and after activities, like vagus nerve stimulation, to see their direct impact on your body.

Work with your coach
Your personal well-being coach will tailor your yōjō journey, turning insights into actions, goals into achievements.

Complete daily tasks
Alongside daily vagus nerve stimulation, you’ll get simple practices — meditation, breathwork, mindfulness, gentle movement — all designed to beat stress and balance your nervous system.
Science
Decades of real-world expertise, powered by science
Everything we do is backed by research, clinical experience, and scientific evidence, and has to survive rigorous review protocols to ensure lasting, positive results.
Pricing
Ready to feel unstoppable?
Just 2 weeks to better sleep — or your money back
£4000+
with yōjō:
£399
90% off
See what’s included with yōjō

£399
90-day money-back guarantee
yōjō taVNS* Device
£299
once-off
Yours to keep
Earpiece
Charger
Conductive gel
Carry case
*Electrical vagus nerve stimulation delivered through the skin of your ear
yōjō Platform
£9.99
/month
First 2 months free
Personalized program
Real-time biofeedback
Personal human coaching
Health education

Your subscription auto-renews after 12 months - £9.99/month or £110 annually upfront.
Cancel anytime and keep your device

Why the Vagus Nerve?
Healthy vagus nerve, healthy you
Relaxation is your body’s preferred state. Stress pulls you out of that state, and the vagus nerve brings you back. A healthy vagus nerve is essential to long-term health and well-being.
Here’s all you need to know about the vagus nerve.
Blog
Explore the science of better living


April 17, 2026
time
-min
read
Acetylcholine: The Resilience Molecule You Can't Afford to Ignore
Serotonin and dopamine get all the attention, but your recovery, inflammation regulation, brain protection, and nervous system flexibility count on this single neurotransmitter most people have never heard of.
You've likely heard of serotonin, the mood molecule. And dopamine, the drive molecule, is very popular. But there's another neurotransmitter that quietly runs the show when life gets hard, and almost nobody is talking about it.
That molecule is acetylcholine, and I'm calling it the resilience molecule.
What is acetylcholine, really?
Acetylcholine (ACh) is one of the oldest neurotransmitters in evolutionary history. It was the first neurotransmitter ever identified, and yet it remains one of the most underappreciated in modern wellness conversations. It was first identified as the driver of muscle contraction, but its role goes far deeper than that.
Acetylcholine is central to memory, focus, heart rate regulation, immune control, mitochondrial function, and the activation of your parasympathetic nervous system. It's the molecule that helps your body recover, adapt, and keep going, hence ‘resilience molecule’.
Where does it come from?
When it was discovered in 1921 by physiologist Otto Loewi, acetylcholine was called vagusstoff (vagus substance). That is because the vagus nerve is its primary delivery system.
Your vagus nerve is the longest cranial nerve in your body, running from your brainstem all the way down both sides of your body to almost every organ, including your heart, lungs, and gut. It uses one motor neurotransmitter when it fires a signal… acetylcholine.
This is the anatomical basis of what researchers call the cholinergic anti-inflammatory pathway.
When the vagus nerve activates, and ACh is released, it binds to alpha-7 nicotinic acetylcholine receptors (α7nAChR) on immune cells. This binding tells macrophages (your front-line immune cells) to shift from pro-inflammatory to anti-inflammatory activity. Inflammation is dialed down, tissue repair up.
This is why vagal tone and heart rate variability (HRV), both measures of how active your vagus nerve is, are so strongly correlated with inflammatory diseases, autoimmune conditions, and recovery capacity.
Low vagal tone means low ACh signalling. Low ACh signalling means chronic inflammation runs unchecked.
ACh and mitochondria
The α7nAChR receptors are not only on immune cells. Research has identified them on the surface of mitochondria, energy-producing structures inside your cells.
When ACh binds to these receptors, it directly supports mitochondrial health and efficiency, which is important because your resilience at a cellular level is tied to how well your mitochondria are functioning.
ACh and brain function
Acetylcholine plays a critical role in two of the brain's most important housekeeping mechanisms: the glymphatic system and microglial cells.
The glymphatic system is the brain's overnight waste clearance network. Sleep architecture — including the cholinergic transitions between sleep stages — shapes when and how effectively this system flushes metabolic waste, including proteins linked to cognitive decline.
When ACh levels and signalling are low, clearance slows, waste accumulates, and brain resilience erodes.
Your brain has its own resident immune cells called microglial cells. ACh regulates microglial cell activity.
Just like the macrophage shift toward inflammation in the body when ACh is low, microglia tip toward chronic inflammation in the brain as well when acetylcholine signalling is low.
A healthy level of acetylcholine regulates inflammation in the brain. Declining acetylcholine is one of the earliest findings in Alzheimer's disease. Supporting ACh today is an investment in a brain that stays sharp for the long haul.
ACh and blood pressure
There's a cardiovascular dimension here, too.
Acetylcholine supports nitric oxide production in the endothelium, the inner lining of your blood vessels. Nitric oxide supports blood vessel dilation, blood pressure regulation, and efficient circulation. This is part of why the vagus nerve is so tightly connected to heart rate variability (HRV), and why HRV reflects overall resilience and nervous system health.
The pattern is consistent.
How to support your acetylcholine levels
This system is highly responsive to lifestyle strategies.
Eat for choline
Acetylcholine is synthesized directly from choline. The richest food sources are egg yolks, beef liver, salmon, and cruciferous vegetables like broccoli.
Most people are not getting enough. The adequate intake is 425–550 mg per day, and surveys consistently show a significant shortfall in the general population.
Support your B vitamins
The methylation pathway, which is essential for choline metabolism and ACh synthesis, depends heavily on B6 (pyridoxine), B9 (folate/folic acid), and B12 (cobalamin).
If you have an MTHFR variant of the enzyme (reductase) associated with B vitamin metabolism, or poor methylation capacity, this may become even more critical in choline metabolism and downstream ACh synthesis — potentially influencing cholinergic signalling and autonomic regulation.
Activate and stimulate your vagus nerve
Since the vagus nerve is the primary driver of ACh release in the body, its health directly determines your cholinergic signalling capacity.
Daily practices that tone the vagus nerve — slow diaphragmatic breathing, cold water exposure, humming, gargling, and singing — will progressively strengthen vagal output and acetylcholine release.
For those who need a more direct intervention, transcutaneous auricular vagus nerve stimulation (taVNS) is an emerging non-invasive tool that directly stimulates the vagal pathway. The stronger your vagal tone, the more readily your body can deploy ACh when it needs to.
Prioritize mitochondrial health
Since α7nAChR is expressed on mitochondria and ACh supports mitochondrial function, a two-way relationship exists.
Anything that supports your mitochondria — quality sleep, cold exposure, time-restricted eating, reduced processed food load — also supports this whole system.
Move your body
Exercise is one of the most powerful upregulators of vagal tone we know of. Resistance training, in particular, has been shown to support acetylcholine signalling at the neuromuscular junction.
Movement is a direct investment in your resilience circuitry.
The gist
Serotonin tells your body you're okay. Dopamine tells your body go and get it. Acetylcholine tells your body to hold together when life gets rough.
Resilience has much more to do with biology than with mindset. And acetylcholine is right at the center of it.
Support your vagus nerve. Eat your choline. Move every day. Take care of your mitochondria.
Your body already knows how to be resilient. Give it the raw materials.

.png)
April 10, 2026
time
-min
read
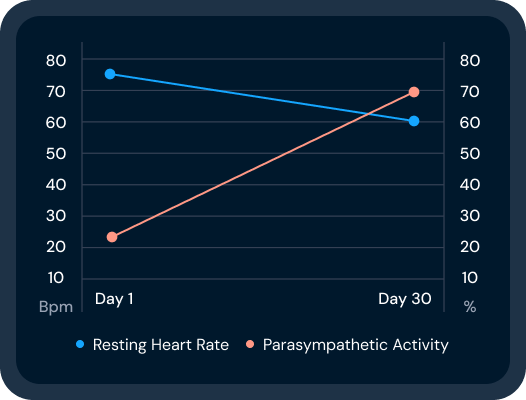
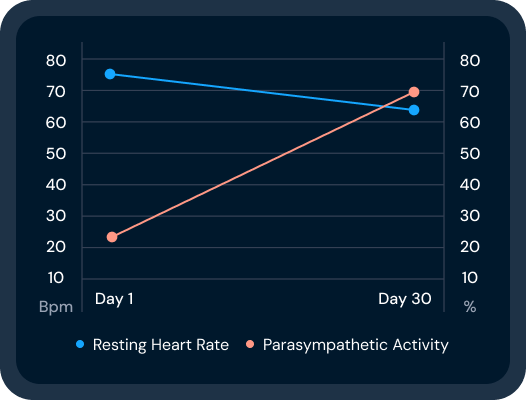
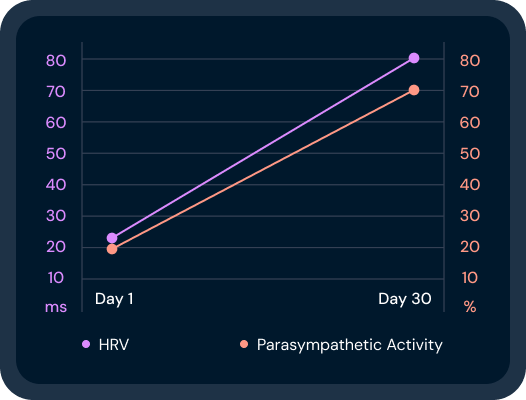
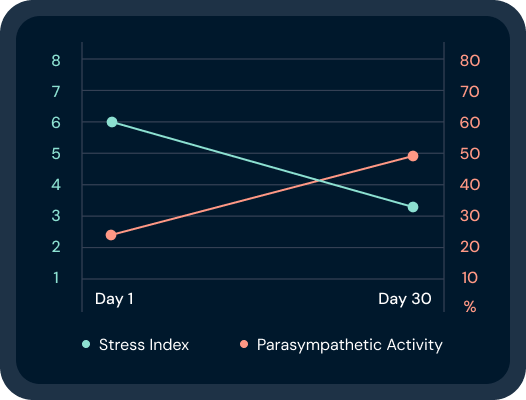
One Low HRV Reading Doesn't Mean What You Think
Your HRV score dipped last night. No sweat. Here's what the science says that dip most likely means.
Your HRV score dropped. Maybe by a lot. You noticed it, and something in you tightened. A small alarm. A question about what you did wrong.
Here is what is almost certainly true: nothing is wrong.
What HRV is actually measuring
Heart rate variability is the difference in time between each heartbeat. It is not a fixed number. It changes constantly.
Your autonomic nervous system controls those beat-to-beat gaps in real time.
Your sympathetic branch is your stress response. It shortens the gaps between heartbeats. It gets you ready to act. Your parasympathetic branch is your rest response. It lengthens those gaps. It drives recovery, digestion, and regulation.
HRV is a live readout of which branch is in charge right now.
Read more about it here.
Why the nervous system varies and why that's the point
The autonomic nervous system is built to shift. It responds to exercise, a stressful meeting, a big meal, a change in temperature, even standing up from a chair.
Research shows that sympathetic activity rises after alcohol, after digestion, after intense exercise, and after poor sleep. All of these lower HRV. None of them mean something is broken.
A healthy nervous system adjusts. It moves toward the stress response when demands rise. Then it returns toward recovery when demands fall. That return is called regulation, and it is trainable.
An unhealthy nervous system gets stuck in stress mode. It loses its ability to recover. Over time, that shows up as a declining HRV trend over time.
One low reading is not the same as a declining trend. The first is normal responsiveness. The second is a sign that recovery capacity may be suffering.
Why a single reading is an unreliable witness
HRV is one of the most sensitive biomarkers available. That sensitivity is also what makes it tricky.
The most common metric in consumer HRV tools is RMSSD. It measures variation between successive heartbeats. It is highly sensitive to noise. Research in HRV methodology shows that even a single irregular heartbeat, or a brief measurement error, can throw off a short-term reading.
In clinical cardiology, the gold standard for meaningful HRV data is 24-hour monitoring. That is because a full day captures the heart's response to a wide range of stimulants and conditions, including natural changes during sleep and activity.
A single reading captures just one small slice of that.
Short readings have their uses. They can show how recovered you are relative to your own normal. But their value comes from tracking many readings over time, and not from interpreting one reading in isolation.
What a low reading is more likely telling you
When your HRV is lower than usual, the most likely explanations are entirely ordinary.
You trained hard recently. Your body is focused on physical recovery. You slept less than usual last night, or your sleep was broken. You drank alcohol, ate a heavy meal, or had a lot of caffeine. You are under a bit of stress — that deadline, that argument, that difficult conversation.
It could even have been your body temperature or posture.
None of these mean your nervous system is damaged. They mean your nervous system is responding to the load. The sympathetic branch is doing exactly what it is supposed to do.
The signal worth paying attention to is what happens over weeks.
A downward trend across multiple readings, taken under normal sleep and reasonable conditions, is worth noticing. A single dip almost always has a simple explanation.
What actually reflects nervous system health
If trends carry the most signal, then the better question is not "why is today's reading low?" It should be "Is my nervous system recovering well across the week?"
It helps to shift our thinking sometimes, especially around health metrics.
Moving our attention away from a number to manage toward a pattern to understand, repositions damage control — trying to keep HRV high — to nervous system care routines.
The autonomic nervous system responds to consistent input. Regular parasympathetic activation, through slow breathing, movement, and non-invasive vagus nerve stimulation, shifts the nervous system's resting state over time.
The one number worth watching
If you track HRV, there is one figure worth more than any individual reading: your rolling average.
Most consumer tools calculate this over a 30, 60, or 90-day window. That number — your personal baseline — is what makes daily changes meaningful.
A reading that is 20% below your rolling average tells you something useful. A reading that matches your baseline confirms normal function. A reading that has been falling for three weeks, across a range of conditions, is worth looking into.
Everything else is your nervous system doing its job.
What this means in practice
One low reading is not a problem to solve.
If your score dropped this morning, start with the simplest questions.
Did you sleep well? Did you drink last night? Did you train hard? Was yesterday stressful? In almost every case, one of those answers explains the reading.
The more useful habit is to notice your trend, track the conditions, and keep doing the things that support recovery long term.
Your nervous system is designed to fluctuate. Let it. Pay attention to where it returns.


Article
March 20, 2026
time
-min
read
How Does Breathing Help the Nervous System?
Breathing is the only autonomic function you can voluntarily control. That's not a small thing.
Who isn’t immediately irritated by the “just breathe” our closest friends and family members take it upon themselves to offer us in times of anger, anxiety, or overwhelm? And when last did you not dismiss it as a well-meaning platitude that didn’t quite reach the depth of what was happening to actually give it a go?
The instruction, it turns out, is physiologically accurate. More physiologically accurate than most of us realize.
Breathing is a primary function of the autonomic nervous system that you can consciously control.
Your heart rate, digestion, and inflammatory responses are not directly accessible, but your breath is. And because it is woven into the architecture of the nervous system at every level, changing how you breathe genuinely changes what your nervous system does.
The nervous system and the breath are inseparable
The brain both produces and listens to breathing.
Research shows that breathing creates rhythms that travel across the entire brain, including areas that have nothing to do with moving air in and out. The brain uses the steady pulse of your breath as a timing signal, keeping different regions in sync, including those involved in emotion, thinking, and memory.
This means the phase of your breath actually changes how your brain performs.
When you inhale, your pupils widen, your reactions speed up, and your ability to form memories improves. When you exhale, those functions ease back down.
Your breath shapes what your brain does next.
The autonomic gateway
Your autonomic nervous system has two main modes.
The first is your sympathetic nervous system, your body’s main stress response. When it activates, your heart rate rises, your muscles tense, and your brain goes on high alert. This is the fight-or-flight response. It evolved to help you survive perceived and physical danger, and it's very good at its job.
The second mode is your recovery mode, your parasympathetic nervous system. This is the state where digestion works properly, sleep does its job, and your body carries out the quiet maintenance that keeps you healthy.
You can't switch directly between these two modes the way you'd flip a light switch, but you can influence which one dominates. And breathing is one of the most direct ways to do that.
Slow, deep breathing turns down the stress response and nudges the nervous system toward recovery mode. This shift is strongest during the exhale. A slow, full breath out is your body's built-in calming mechanism.
The reverse is also true.
Fast, shallow breathing keeps the stress response running. Your nervous system reads it as a signal that something is still wrong.
The breath and the stress response feed each other in both directions.
Which means you can interrupt the cycle whenever you want.
Need more energy? Quicken your breath. Feeling a wave of anxiety? Slow down and deepen your breathing.
The vagus nerve: the calming pathway
The vagus nerve is the main information highway of your parasympathetic nervous system, the system responsible for rest and recovery. It runs from the brainstem all the way down through the heart, lungs, and gut. It carries signals in both directions. What most people don't know is roughly 80% of your vagus nerve’s signals travel upward, from the body to the brain.
Your brain listens to your body through this nerve.
When you take a deep breath, your lungs expand. That expansion activates tiny pressure sensors embedded in the lung tissue. These sensors send a signal up through the vagus nerve to the brainstem, activating parasympathetic responses.
That's not a small thing. A slow, deep breath is a direct input into one of the most important nerve pathways in your body.
This is why breathwork is a big part of yōjō's approach to nervous system regulation.
Breathing and the brain
The effects of breathing extend well beyond the autonomic nervous system.
Quieting the amygdala
When you're anxious or have been going through a long period of stress, your brain becomes electrically overactive. The nerve cells in areas of your brain that process emotions start firing more than they should, especially in the amygdala, the part of the brain that detects threats and triggers fear responses.
Slow, deep breathing is thought to help counteract this through a process called cellular hyperpolarization.
Cell-to-cell communication is like a domino effect. A signal passes from one cell to another through changes in each cell's electricity. If the cells are very excited, they are more likely to pass on the signal. A hyperpolarized cell is less excited. Its electrical potential is more negative, and it is less likely to pass on a signal.
This theoretical framework suggests that the quieting effect of hyperpolarization is particularly strong in the amygdala and thalamus. Processing fear and emotions, hyperpolarization in the amygdala and thalamus reduces anxiety and dampens negative emotional states.
Far from just relaxation in the everyday sense of the word, the effect of breathing on the brain is measurable. Breathing directly influences your threat-detection system.
GABA and rest
Your brain has a natural calming chemical called gamma-aminobutyric acid, or GABA for short.
GABA's job is to reduce overactivity in the brain. When GABA levels are healthy, the nervous system is better able to settle down, sleep properly, and manage stress. When GABA levels are low, the opposite tends to happen — anxiety increases, sleep suffers, and the stress response becomes harder to regulate.
Research has shown that breathing practices can increase GABA activity in the brain.
This is part of why consistent breathwork tends to build up gradually rather than provide momentary relief. Each session shifts your brain's baseline chemistry toward a more regulated state.
BDNF and neuroplasticity
Your brain is constantly changing. It grows new neurons and repairs existing ones to keep your nervous system adaptable. To do this, your brain relies on a growth protein called brain-derived neurotrophic factor, or BDNF.
BDNF is like a fertilizer for your brain, and higher concentrations of it are linked with better learning, improved mood, and greater resilience to stress.
Some breathing interventions have been indirectly linked to increases in BDNF. Preclinical trials indicate that vagus nerve stimulation can lead to an increase in BDNF, and some breathing techniques do activate the vagus nerve.
So, it isn’t a great leap to suggest that breathing can increase BDNF levels. This means breathwork can create the biological conditions needed for the nervous system to change, to become structurally more resilient.
Resetting chronic patterns
Perhaps the most important finding in this area of research is what happens when breathwork becomes a consistent habit.
Chronic stress doesn't just make you feel bad in the moment. Over time, it rewires your brain. Your nervous system starts to treat high alert as its default setting, even when there's no real threat around. The patterns of activation that were once a stress response become your baseline state.
This helps explain why so many people struggle with persistent anxiety, low mood, disrupted sleep, or difficulty bouncing back from stressful events. It is a feature of the modern world: our nervous systems have been gradually shaped by repeated stress and have settled into those grooves.
Intentionally changing your breathing patterns can disrupt the groove digging, helping your brain reset.
Research suggests this goes beyond temporary relief.
Consistent breathwork may produce lasting changes in how strongly neurons connect and in the nervous system's flexibility, its ability to return to a state of balance after stress.

FAQs
Got questions? We’ve got answers.

M.D., Ph.D., FASRA
Chief Medical Officer
Professor Emeritus of Anesthesiology, Orthopaedics, and Pain Medicine at the University of Florida College of Medicine, Boezaart has 35+ years of clinical expertise and champions evidence-based, person-focused strategies to improve quality of life.













.webp)
.webp)














.webp)