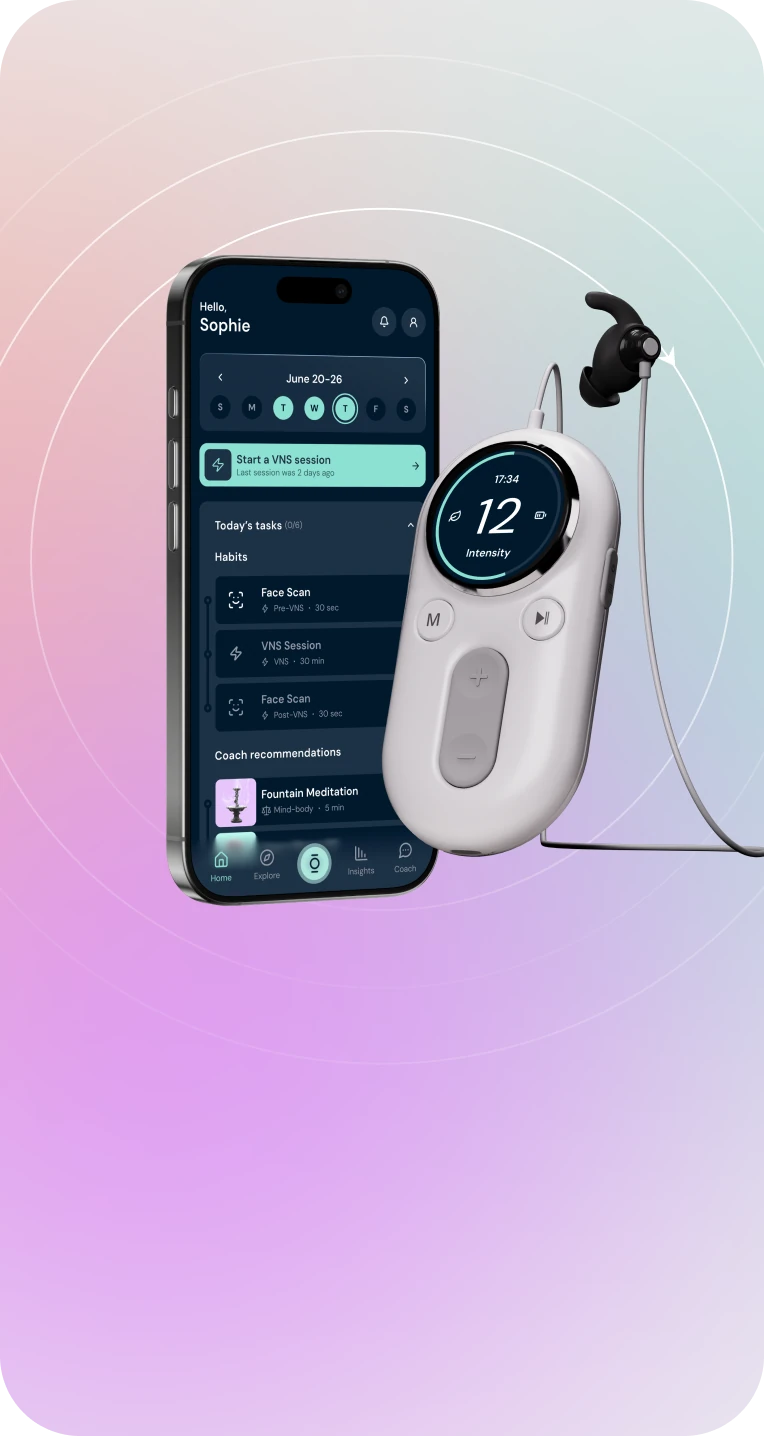

We make VNS a sustainable habit
yōjō is your daily nervous system reset for better sleep, faster recovery, sharper focus, deeper calm, and more energy.


Accurate, effective, consistent VNS
Modern life keeps us in stress mode, unbalancing the autonomic nervous system. This affects sleep, focus, mood, and energy, and increases inflammation, anxiety, and pain.
Vagus nerve stimulation (VNS) restores balance… but only if done daily.
yōjō helps you turn vagus nerve stimulation into a daily habit so you can get the most out of it.
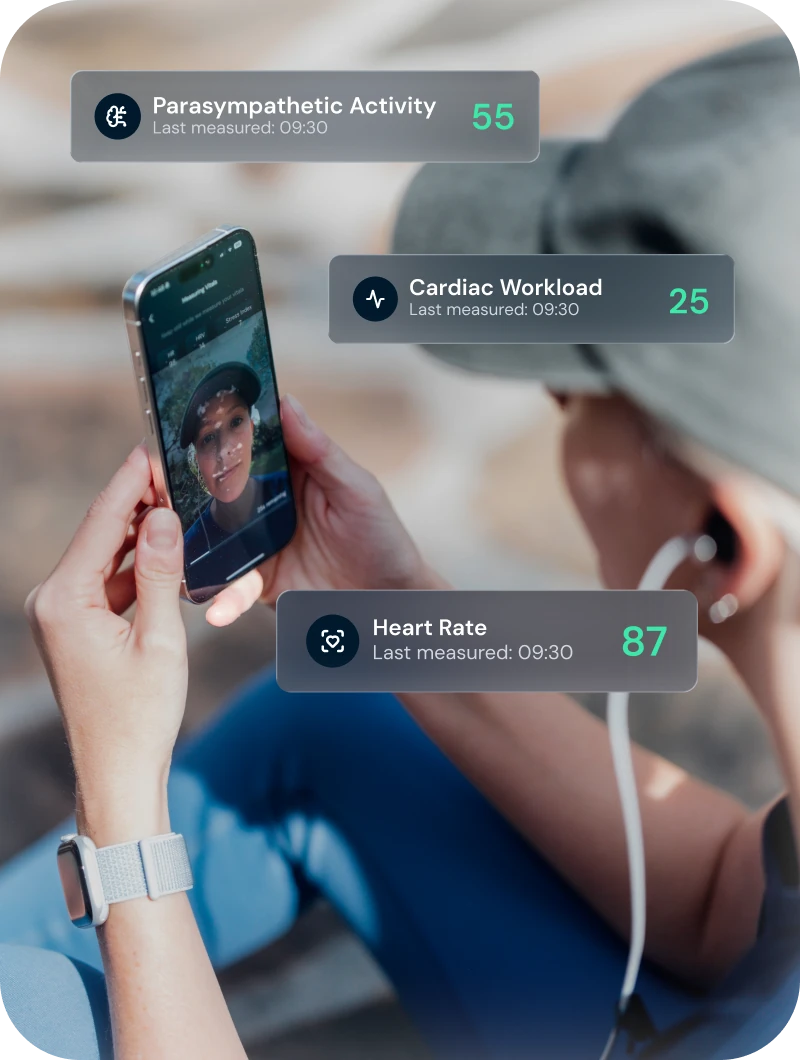
Our whole-person approach combines a premium stimulator, health metrics face scan technology, real-time biofeedback, and expert human guidance to make nervous system balance as automatic as brushing your teeth.

yōjō vs. Pulsetto vs. Nurosym
Why yōjō?
Where most VNS companies stop at stimulation, yōjō combines behavioral science, biofeedback, and human guidance to turn daily vagus nerve care into a life-changing habit. Here’s how yōjō compares with Pulsetto and Nurosym.

Difference
Your everyday
vitality, supported
A full system that helps you get the most out of vagus nerve stimulation… and life.
Testimonials
Real people, real impact
What yōjō members say a few weeks after making yōjō a part of their daily routine.

How It Works
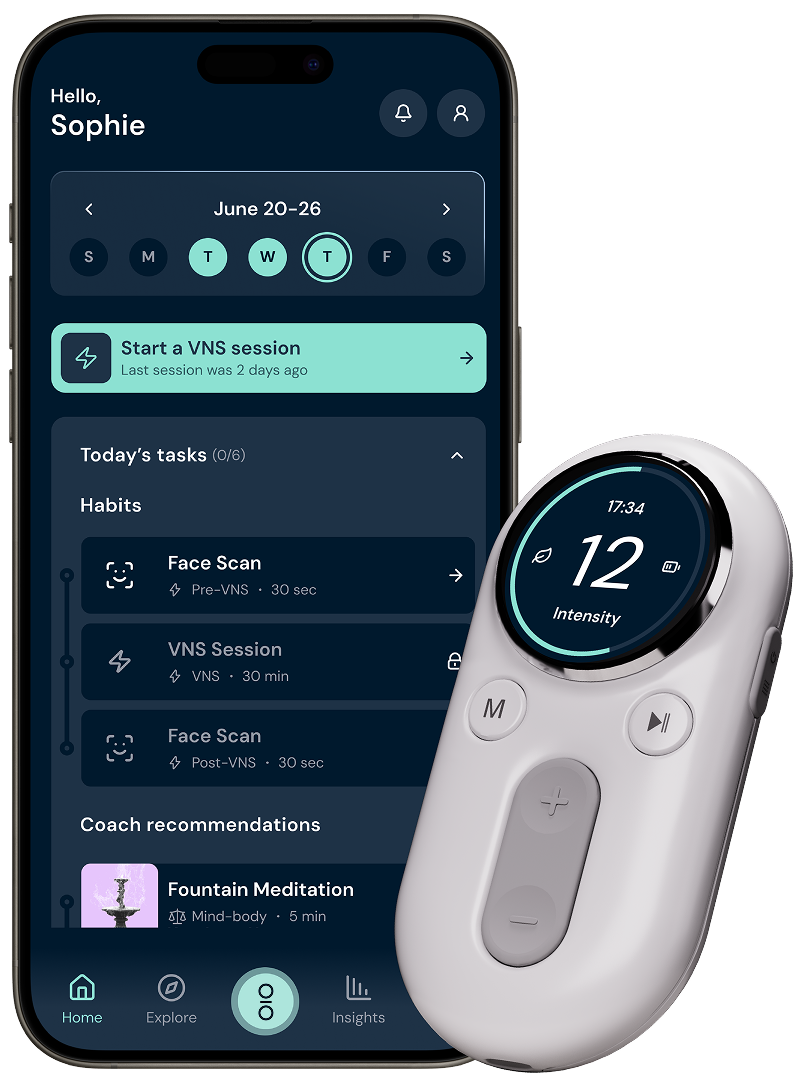
A small daily ritual that helps you do you, better
The yōjō vagus nerve stimulator and app work together to give you the stimulation, data, and guidance you need for long-term vitality.

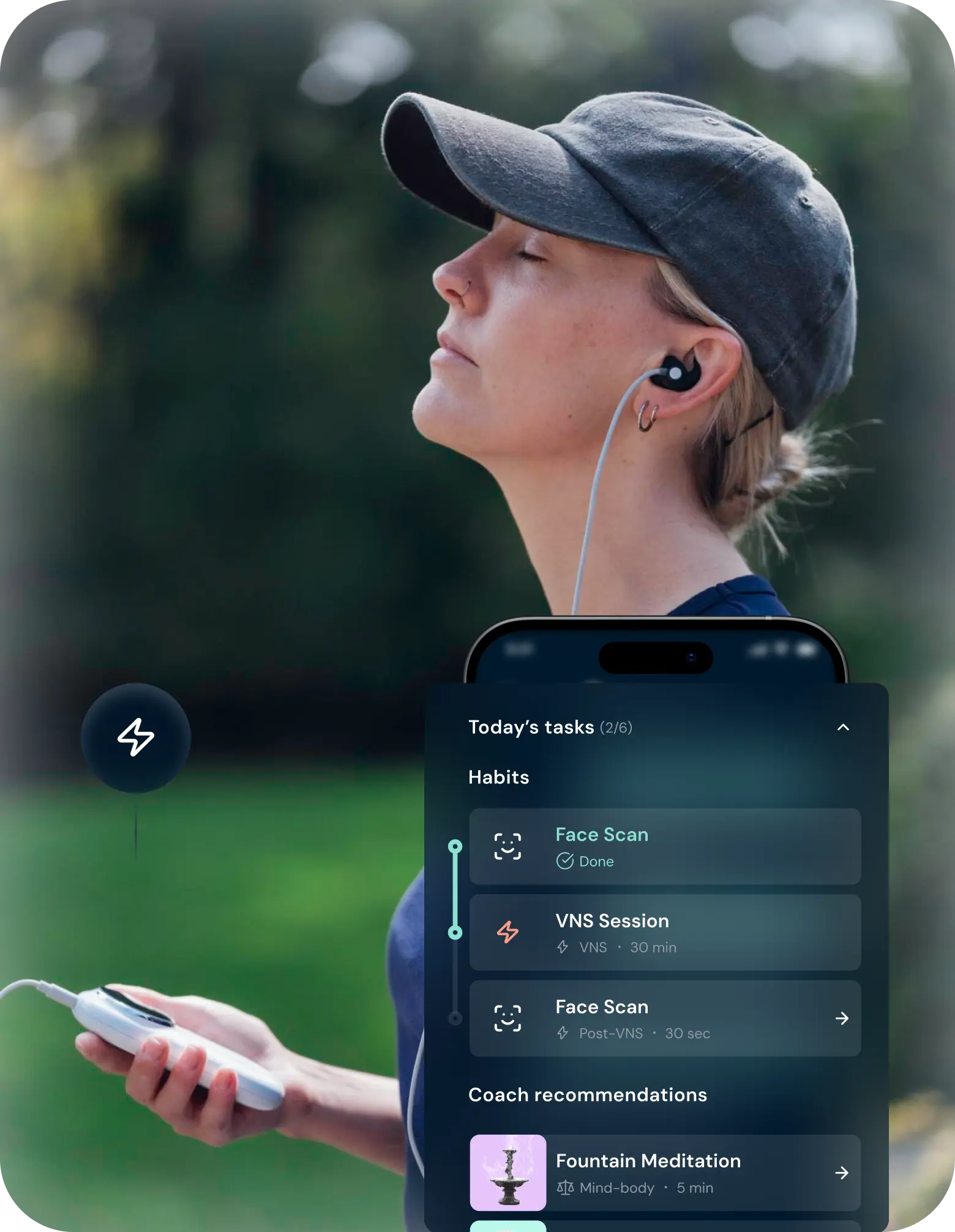

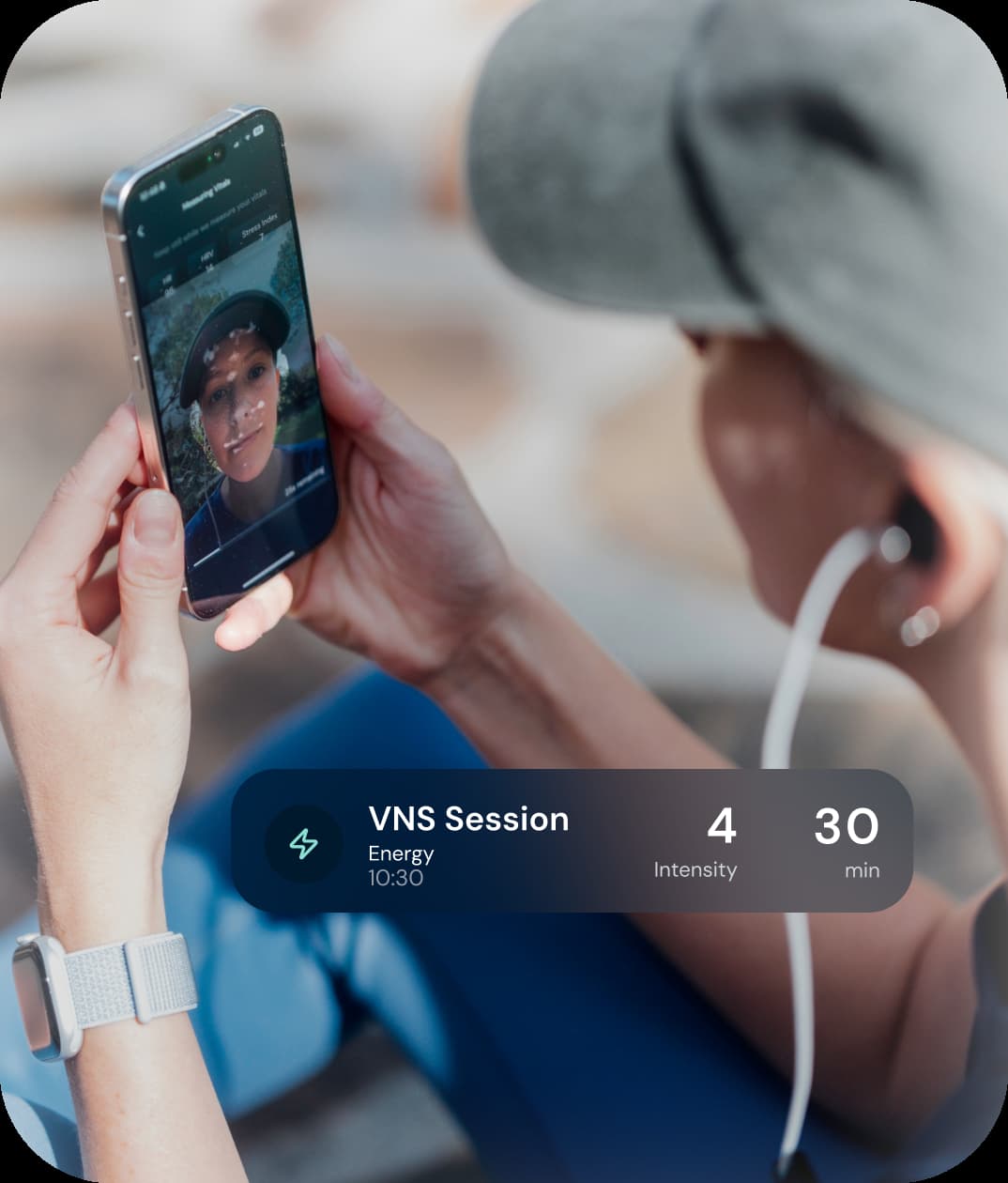
Scan
Capture pre-session metrics through a 30-second selfie.
Session
Complete a 30-minute ear-based vagus nerve stimulation session. Completely hands-free.

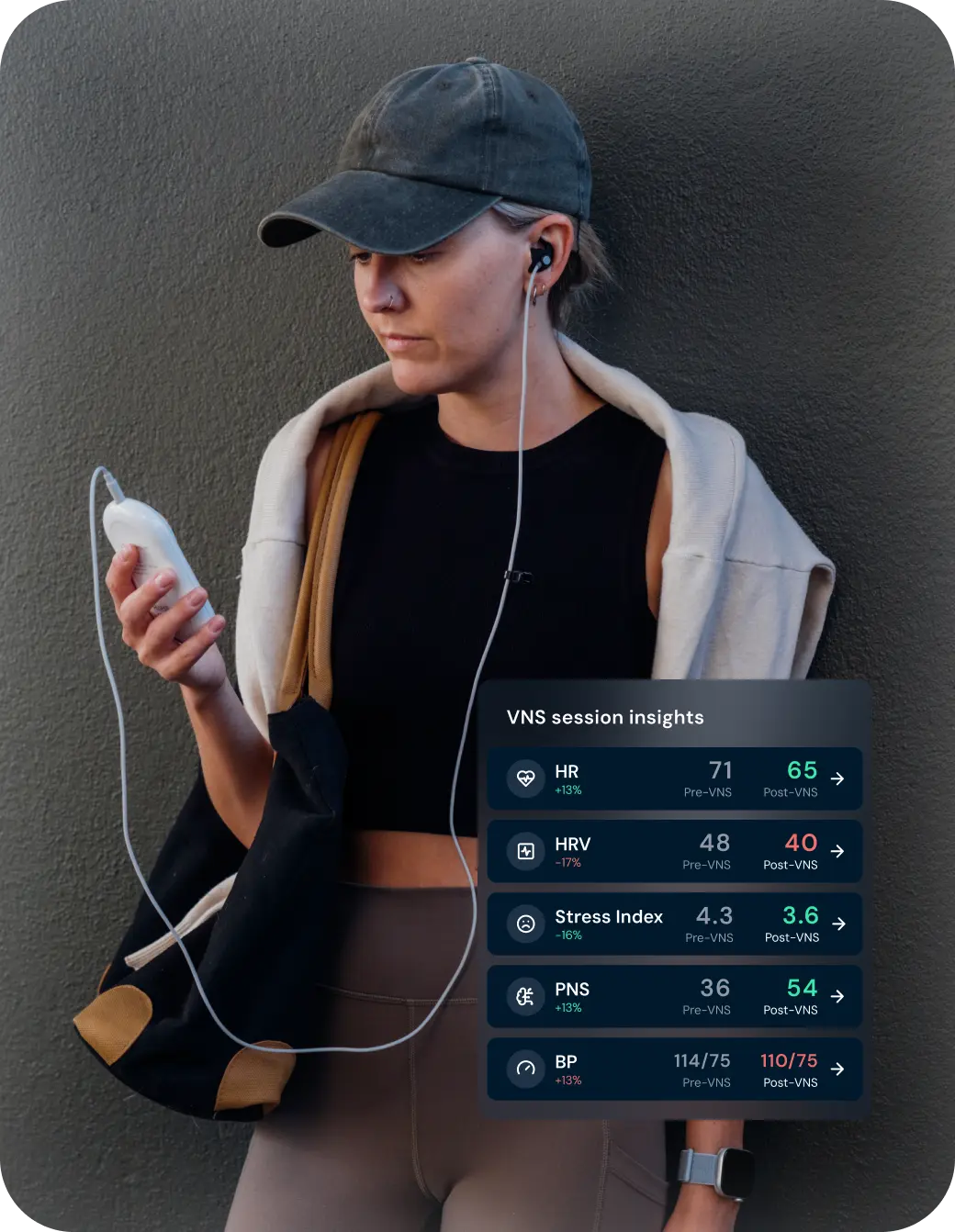
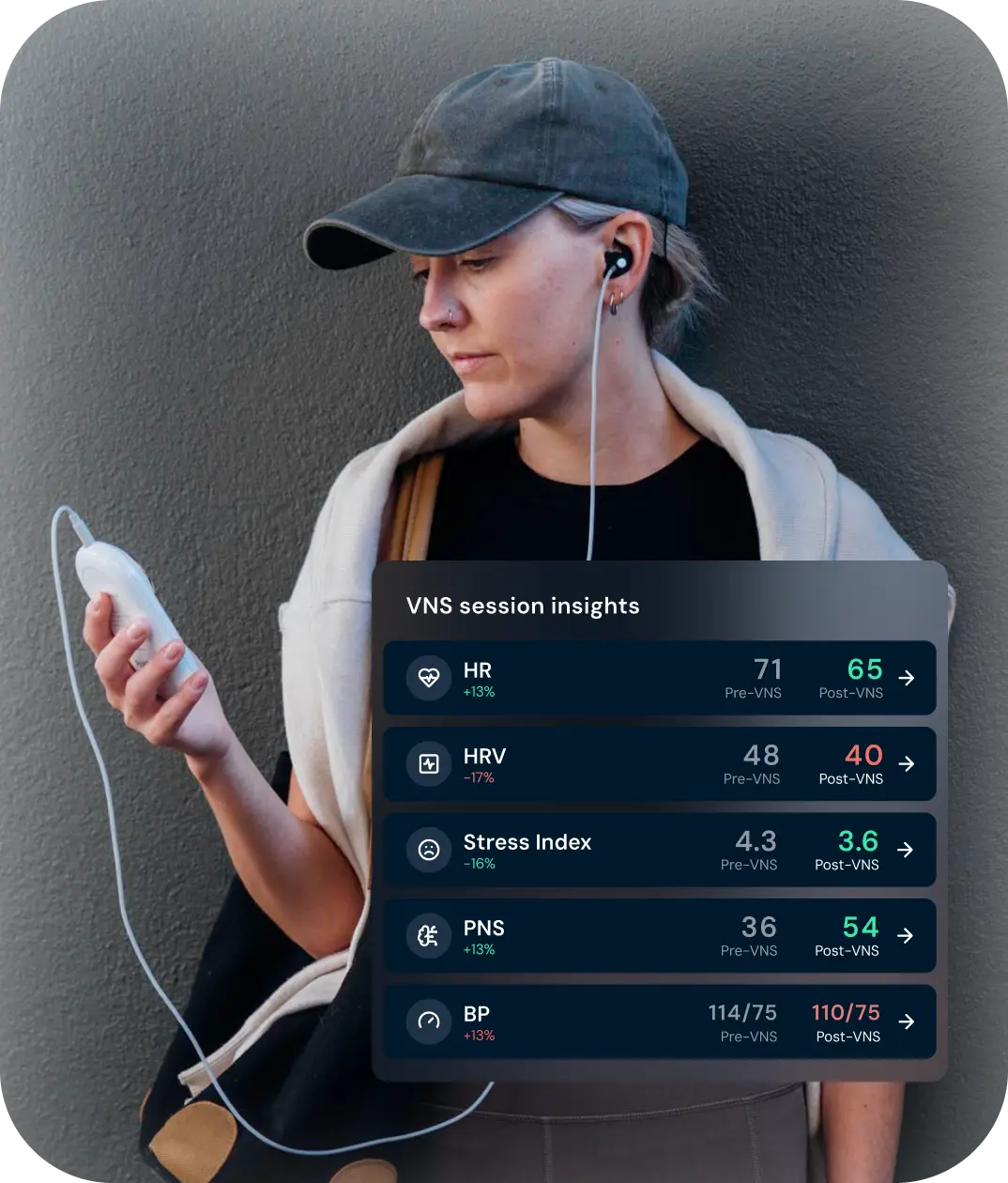
Result
Capture post-session metrics and see the session’s impact on your nervous system balance.
Pricing
Ready for superior vagus nerve care?
Just 2 weeks to better sleep — or your money back
£4000+
with yōjō:
£399
90% off
See what’s included with yōjō

£399
90-day money-back guarantee
yōjō taVNS* Device
£299
once-off
Yours to keep
Earpiece
Charger
Conductive gel
Carry case
*Electrical vagus nerve stimulation delivered through the skin of your ear
yōjō Platform
£9.99
/month
First 2 months free
Personalized program
Real-time biofeedback
Personal human coaching
Health education

Your subscription auto-renews after 12 months - £9.99/month or £110 annually upfront.
Cancel anytime and keep your device

Blog
Explore the science of better living


Article
May 8, 2026
time
-min
read
My yōjō Journey and What I Didn’t Expect
When I first started using yōjō back in December, I approached it the way I approach most wellness tools: open-minded but measured. Here’s what happened.
As a GP, I understand the science behind vagus nerve stimulation. I know the vagus nerve is the body’s master regulator, that it connects the brain to the body, and that it governs that all-important shift from ‘fight-or-flight’ into ‘rest-and-digest’. I know the mechanism, but I don’t think I really expected the impact.
I definitely wasn’t prepared for how much of a difference I would feel.
How I yōjō
My routine is simple.
Every night, when I go to bed, I grab my yōjō. I apply the gel to the earpiece and pop it in my ear. I find a comfortable intensity and then just let the gentle electrical pulses do their thing.
I also use it during the day when I remember. This is becoming more frequent because the benefits have become harder to ignore.
The sensation took a little getting used to — little electrical zaps that you have to set to your comfort level — but it quickly became something I looked forward to rather than something I had to remind myself to do.
What surprised me most
Sleep. Sleep. Sleep.
I’ve always been someone who can lie awake, mind whirring, tossing and turning for hours before finally dropping off. In the first few days of using yōjō, I noticed I was falling asleep faster.
At first, I put this down to coincidence, a good few days, or a placebo effect. But now, several months in, I can say with confidence that it is none of these.
On the nights I use yōjō versus the nights I don’t, there is a noticeable difference.
My Garmin data backs this up, too: sleep quality has genuinely improved, not just my perception of it. And that matters to me as someone who values having objective data alongside improvements in how I feel.
Getting to sleep faster has been the biggest win.
Anyone who knows that particular frustration of lying in the dark, wide awake, brain refusing to switch off, will easily understand just how significant this has been.
A shift in how I think about my nervous system
Something I didn’t anticipate was how using yōjō would make me more intentional about my parasympathetic nervous system more broadly.
Understanding something intellectually and actively working on it are two different things. yōjō has brought vagal tone into my daily awareness in a way that’s spilled over into other habits.
I now use the physiological sigh regularly — a double inhale through the nose followed by a long exhale — which is one of the fastest ways to manually activate your parasympathetic nervous system. It’s the kind of technique I’ve always known about, but yōjō has made me more motivated to layer these practices together.
I feel more in control of my own nervous system regulation, and that feeling of agency is something I hadn’t expected to value as much as I do.
Would I recommend it?
I started this journey curious. I’m continuing it as a genuine convert.
Whether you’re someone who struggles to wind down at night, feels chronically overstimulated, or simply wants to feel more grounded in your own body, yōjō offers something that is both accessible and, in my experience, genuinely effective.
The science was always there. And now I’ve felt it for myself.


Case study
May 11, 2026
time
-min
read
Beyond endurance: yōjō x gROW Atlantic
ANNOUNCEMENT: yōjō and gROW Atlantic have partnered for the World’s Toughest Row 2026. Will on-the-go autonomic care boost endurance?
A few months ago, the gROW Atlantic Team, Vicki Anstey and Dr. Sophie Bostock, asked us a simple question: could yōjō help the team not only survive crossing the Atlantic in a row boat but make it across faster than any other female team?
We said we think so, let’s see.
This December, Vicki and Sophie will join the World's Toughest Row 2026: a 3,000-mile rowing race starting in San Sebastian, La Gomera, Canary Islands and ending at Nelson's Dockyard, Antigua. They're aiming to break the current world record for a female pair — 38 days and 12 hours — rowing two hours on, two hours off, for an estimated 1.5 million oar strokes.
They’ll face storms, salt, and silence. Sleep deprived and alone, they’ll have no support boat alongside them, no shore team, and no shortcuts — just two athletes, an ocean, and whatever they have brought with them, which happens to include their yōjōs, because peak performance, rapid recovery, and sustained endurance come from a well-regulated and flexible nervous system.
Meet the record-breakers
Vicki is a world record-breaking adventurer, TEDx speaker, and a leading expert on resilience, mindset, and human performance. She is a Certified Stress & Resilience Coach, UK Ambassador for Inspiring Girls, and one of the first women finalists on Channel 4's SAS: Who Dares Wins. She holds two world records for rowing the Pacific Ocean unaided in 2021 and for cycling 3,000 miles across America in the 2024 Race Across America.
Sophie is a sleep scientist with a PhD, the founder of The Sleep Scientist, and a national authority on sleep, recovery, and the nervous system. She has worked with elite athletes, surgeons, military personnel, and Olympians on the science of rest, alertness, and resilience under pressure.
Between them, they hold decades of expertise in the exact systems yōjō exists to support: rest, recovery, regulation. Which is what makes this partnership feel so natural.
No strangers to nervous system health, Vicki and Sophie have been thinking about, teaching, and living autonomic flexibility long before they ever set foot in an ocean rowing boat.
What their bodies will face out there
It’s called the World’s Toughest Row for a reason.
More people have climbed Everest than have rowed across an ocean. For a two-person crew, the load is particularly unforgiving. There is no third pair of hands. If one of you is sick, injured, or simply exhausted, the other one rows.
To understand why this matters to us, it helps to understand what around 38 days of that environment does to a human nervous system.
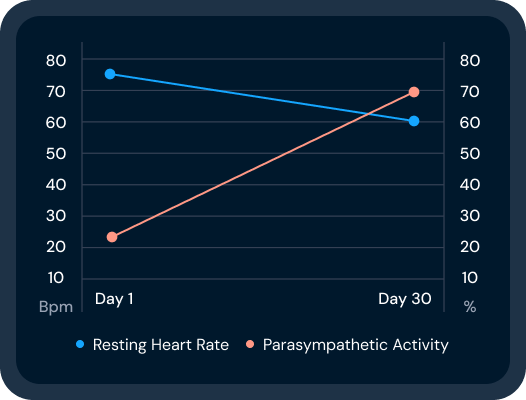
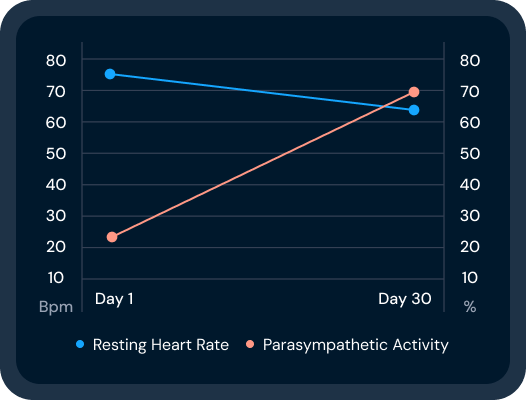
The autonomic nervous system has two branches that work in balance. The sympathetic branch drives action, picking up heart rate, quickening breathing, elevating cortisol levels, and narrowing attention. The parasympathetic branch, carried largely by the vagus nerve, does the opposite. It slows the heart, deepens the breath, and shifts the body into the state where repair, digestion, and recovery happen.
In healthy daily life, these two branches alternate fluidly. You activate when you need to act. You recover when you don't. That flexibility — the ability to shift between drive and recovery on demand — is what we mean by autonomic balance, and it shows up in measurable signals like heart rate variability (HRV).
Ocean rowing collapses that flexibility.
Sleep is fragmented into 90-minute windows (usually less!), never allowing a full recovery cycle. Rowing through the night completely disrupts circadian rhythms. Cortisol stays elevated. Cold and salt exposure keep the sympathetic system primed. Caloric deficit and dehydration add further stress signals. The body, in short, is held in a state of near-continuous sympathetic activation for six weeks. Unfaltering stress.
When the dominant state will be one of stress, could parasympathetic support give Vicki and Sophie the snatches of recovery they need precisely when they need it?
Where we come in
yōjō exists for one reason: to help people maintain autonomic flexibility — the ease with which the nervous system shifts between drive and recovery. We do that by supporting parasympathetic activity through daily vagus nerve stimulation, human coaching, and data-driven personalized programs.
For Vicki and Sophie, who are about to test their nervous systems under conditions that compress years’ worth of physiological stress into 6 weeks, yōjō will be providing on-the-go access to their parasympathetic systems and a way to boost nervous system recovery through the full arc of this journey.
That means yōjō devices on board, with daily vagus nerve stimulation built into their training and racing routines. It means personalized protocols, tuned to each athlete's physiology, training load, and recovery profile. It means ongoing science support, from prep to finish, our science team reviewing data, iterating protocols, and answering the questions that come up along the way.
This is the cleanest possible expression of the science we build around. Helping two of the most physiologically literate athletes access recovery under conditions designed to deny it to them is precisely what yōjō is here to do.
Follow along
This is the start of an eight-month journey that will end on a beach in Antigua in early 2027. Between now and then, we'll be sharing the science, the milestones, and the data from Sophie and Vicki’s first training rows to their return to life after the race, and will be digging much deeper for a three-part documentary series called Do you, better.
If you want to follow along on LinkedIn and Instagram, we'd love to have you.


Article
May 1, 2026
time
-min
read
What Allostatic Load Actually Is and Why You Can't Push Through It
I sleep fine, but I’m still exhausted. What’s up? Allostatic load, that’s what.
There is a particular kind of exhaustion that sleep doesn't fix. We all feel it. Taking time off to rest doesn’t help. Sipping the air along the coast doesn’t replenish. Reading under a willow tree and listening to a whip-poor-will brings only momentary lightness. Every day begins with dread and ends with another well, at least we got through it.
Who can be blamed for turning on oneself?
Is this another failure of mine? Is it a discipline problem? Is it a matter of better time management or positive thinking? Is it because I walked under a ladder that one time? Do I lack grit?
No.
In this case, what feels like a willpower problem is more often a physiological one. And at its center is something called “allostatic load”.
What is allostasis
Allostasis is your body’s adaptive system. It maintains stability through change.
The baseball player out in left field who has sensed something in the body language of the batter starts to jog forward, his eyes locked on the ball flying from the pitcher’s hand. When the ball eventually pops up into the air, the player is already in motion, already underneath it, mitt reaching. This is allostasis.
Allostasis is your body predicting demands and preparing for them. It is why you begin to shiver when you step into cold air — your body has sensed the change in environment, knows a sudden drop in body temperature is possible and dangerous, and so rapidly contracts and relaxes your muscles to generate heat.
Prediction and preparation. The aim is homeostasis — internal balance.
This makes allostasis extraordinarily effective under normal conditions. The problem is what happens when those conditions are no longer normal.
What happens to the game if, after catching the ball and tossing it back to the pitcher, the baseball player does not return to his original position and instead runs around after imaginary fly balls?
Where the system begins to fail
There is a physical cost to allostasis. Changing bodily processes and triggering actions to pre-emptively maintain homeostasis have consequences. If allostatic processes are activated too often or stay activated for long periods, these consequences accumulate.
Called allostatic load, this accumulation leads to inadequacy and dysfunction.
If an allostatic process is activated frequently and never shuts off, eventually the changes it affects will grow less and less appropriate, its abilities to respond to anticipated needs stunted.
Your body, still driven by the need for homeostasis, sets other allostatic processes going to compensate.
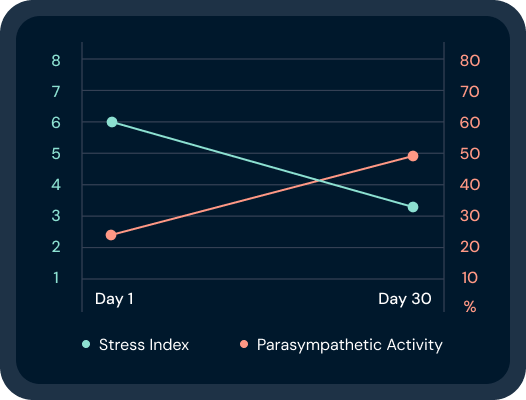
Allostatic load is very obvious in chronic stress.
Your stress response is fundamentally allostatic and can cause a lot of damage if it becomes dysregulated.
Stress and allostatic load
During a stress response, your body releases adrenaline, cortisol, and pro-inflammatory cytokines. These are not inherently harmful. In the context of a brief, genuine threat, they are precisely what keeps you alive.
Adrenaline sharpens focus and mobilizes energy. Cortisol sustains the response and modulates immune function. Pro-inflammatory cytokines coordinate the immune system's rapid activation.
Duration is the problem.
When cortisol remains chronically elevated, your cells begin to downregulate their sensitivity to it, a biological response to over-signaling. The immune system, which normally depends on cortisol as a brake, begins to lose that brake. The result is immune dysregulation, which typically manifests as chronic low-grade inflammation.
Chronic inflammation is thought to weaken the lining of your gut, weakening the barrier between your gut and your bloodstream. Inflammation also spreads like a rumor, only deepening the problem. Chronic stress is widely accepted as a major driver of noncommunicable conditions such as metabolic syndrome, cardiovascular disease, type 2 diabetes, chronic pain, and neurological conditions, including depression. A large UK Biobank study published in 2025, drawing on data from over 200,000 adults, found that allostatic load independently predicts cardiovascular risk.
This is how chronic stress becomes structural illness. And it isn’t your fault.
Why modern stress is a particular problem for this system
Your allostatic system evolved for a different threat landscape.
A predator appears. Adrenaline spikes. Cortisol sustains the response. You flee, or you fight. The threat resolves. The parasympathetic nervous system re-engages. Cortisol clears. The system resets.
The entire sequence from activation to recovery might take minutes.
Modern psychological stressors, however, seem never to resolve.
A difficult conversation with a manager, a delayed email, anxiety about financial instability, and low-level dread about the news all trigger your allostatic stress response. But then your body never gets the signal that the threat has passed. There’s always another email.
Whether the threat is a predator or a deadline, both converge on the same downstream stress response: the same hormones, the same physiological activation, the same suppression of recovery. Allostatic load is the result of an ancient adaptive system confronting conditions it was never designed for.
And you can feel it.
Wired by tired. Non-restorative sleep. And even the self-loathing, which one meets with the mantra of the modern world: work harder.
Why you can’t push through the accumulated load
The dominant cultural response to stress is effort.
“When the going gets tough, the tough get going”.
Work harder, focus more, manage time better. Sleep when you’re dead.
This response makes intuitive sense if stress is understood as a performance or discipline problem.
It is exactly the wrong response if stress is understood as a physiological state. This is what people often get wrong about burnout. They miscategorize it and so mistreat it.
When allostatic load is low, the stress response is appropriately calibrated. You engage, you recover, you adapt. This is what the system is designed for.
When allostatic load is high — when the failed shut-off pathway has been running for months, when inflammation is chronically elevated, when cortisol sensitivity is impaired — the system is already dysregulated.
Pushing harder does not clear the load. It adds to it.
When a system designed for recovery is never given the conditions to recover, trying harder means feeling worse.
What recovery actually means in this context
To reverse allostatic load, you need to allow your parasympathetic nervous system space and time to do its job. And this is why the vagus nerve is getting more focus these days.
It is the primary arm of your parasympathetic nervous system. You can read more about ‘The Wanderer’ here. Activating the vagus nerve more regularly provides that parasympathetic moment. Slow deep breathing activates the nerve, particularly extended exhalation.
Sleep is also helpful as it is the primary window during which cortisol clears and inflammatory markers reduce.
Social safety and perceived control appear to reduce the frequency of allostatic activation in the first place. The more often you’re around people you trust in environments you know, the less primed you are for predict and prepare.
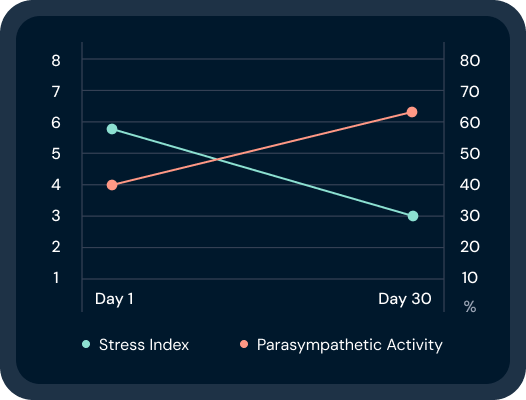
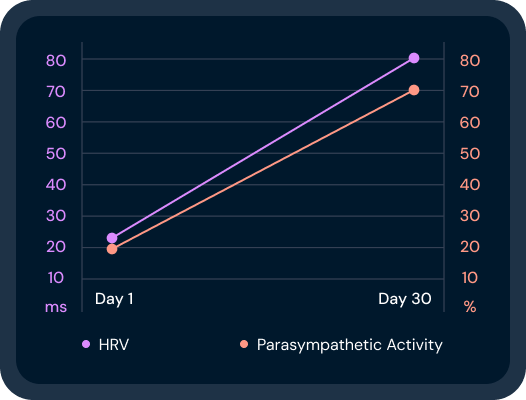
Heart rate variability, or HRV, is one of the cleaner signals of whether you’re accumulating allostatic costs or shedding them.
HRV reflects the dynamic balance between stress and relaxation activity — a measure of how flexibly your autonomic nervous system responds rather than how rigidly it holds a fixed state.
Research shows that HRV declines with increasing allostatic load. Improving vagal tone and HRV over time may help reverse allostatic load, but the link is tenuous and an active area of research.
What now?
The person who turns on themselves — who counts the ladders they've walked under, who wonders if it's a grit problem — is not weak. They are doing the only thing that makes sense when no one has explained the biology.
Now you have a better explanation.
Allostatic load is real, it is measurable, and it responds to the right conditions. The body that accumulated it is the same body that knows how to recover from it. It just needs to be given the chance.
Give your body a chance with yōjō.

FAQs
Got questions? We’ve got answers.

M.D., Ph.D., FASRA
Chief Medical Officer
Professor Emeritus of Anesthesiology, Orthopaedics, and Pain Medicine at the University of Florida College of Medicine, Boezaart has 35+ years of clinical expertise and champions evidence-based, person-focused strategies to improve quality of life.


.webp)
.webp)
























.webp)